In this article, we explain what medical professionals understand by a “prolapse” and what types of prolapse there are. A prolapse can affect various organs and body regions. As a rule, it is accompanied by high or incorrect loads and/or signs of wear. Age, genetic predisposition and lack of exercise also promote prolapse.
Definition of prolapse
The term “prolapse” comes from the Latin term “prolapsus” and means “incident”. This literally means that something in the body falls out of its healthy position, i.e. shifts pathologically. Another common term for prolapse is “lowering.” However, this refers to the fact that an organ lowers downwards, but without completely stepping outwards. Organ prolapse is therefore the precursor of the total prolapse of an organ.
Common types of prolapse include:
- Disc prolapse (herniated disc of the spine)
- Uterine prolapse (uterine prolapse)
- Vaginal prolapse (vaginal prolapse and vaginal prolapse)
- Hemorrhoids and prolapse
- Rectal prolapse (prolapse of the rectum)
Organ prolapse plays a special role in women’s health.
Organ prolapse in the female body
Especially after childbirth and with increasing age, women are at risk of excessively lowering organs of the abdomen (the pelvic organs, bladder and uterus). The reason for this is damage to the supporting apparatus caused by the strenuous birth process, damage to the nerve tracts, genetic or age-related connective tissue weakness and weak pelvic floor muscles.
Lowering of the abdominal organs is a natural process that affects about half of all women in the course of their lives. They require medical treatment only in the case of clear symptoms and total prolapse, often they even remain undetected.
Lowering and prolapse of the vagina

Prolapse and prolapse of the female genitalia can be differently pronounced and affect various abdominal organs. The mere lowering of the vagina and uterus is not externally visible and is noticeable for the patient as an unpleasant feeling of pressure in the area of the vagina and bladder. This pressure can lead to urinary urgency and uncontrolled urinary and defecation. This is unpleasant, but often does not require treatment. The symptoms usually disappear completely overnight due to the changed body position.
Due to the non-specific symptoms of genital prolapse, it is often only the gynaecological examination that leads to a diagnosis of vaginal prolapse or uterine prolapse. If there is a suspicion of lowering of the uterus or female genital organs, the following symptoms are particularly noticeable:
- A feeling of pressure downwards
- Pain in the vagina and/or coccyx
- The bladder feels constantly filled
- Incontinence during stress (sneezing, coughing, etc.)
- Complaints recede at night
Doctors only speak of a vaginal prolapse when the vaginal prolapse becomes visible at the vaginal opening, i.e. the mucous membrane of the vagina shows up there. In such a fulminant vaginal prolapse, the involvement of other organs (bladder, intestine) can occur due to the pronounced protuberance. Then palpable swelling forms in the upper or lower part of the vaginal opening.
If it comes to the exit of the uterus from the vagina, then a doctor recommends appropriate treatment in individual cases. For example, a silicone pessary can be inserted into the vagina to replace the supporting function of the pelvic floor and the holding apparatus. Surgery or removal of the uterus (hysterectomy) is also possible. Which therapy promises healing depends on the suffering, symptoms and the status of the family planning of the affected patient.
Prevention of uterine prolapse
The uterine prolapse is usually not very painful and does not necessarily lead to the more severe impairments, even if patients often fear this. Rather, uterine prolapse is a completely natural process. It is caused by the weakening connective tissue with age, the physical strains of natural birth, the sagging ligaments and fascia as well as the neglected muscles of the pelvic floor.
The pelvic floor consists of three muscle layers, ligaments and connective tissue. In order to prevent progressive uterine prolapse and ultimately the threat of uterine prolapse, health experts recommend regular pelvic floor exercises or regular pelvic floor training. Because the pelvic floor supports the organs of the abdomen (bladder, vagina and uterus) like a hammock. At the same time, it ensures the control of bowel and urinary discharge.
A trained pelvic floor should not only prevent organ prolapse in women and help against incontinence, but should also give people of all genders a more fulfilling sex life.
Pelvic floor exercises
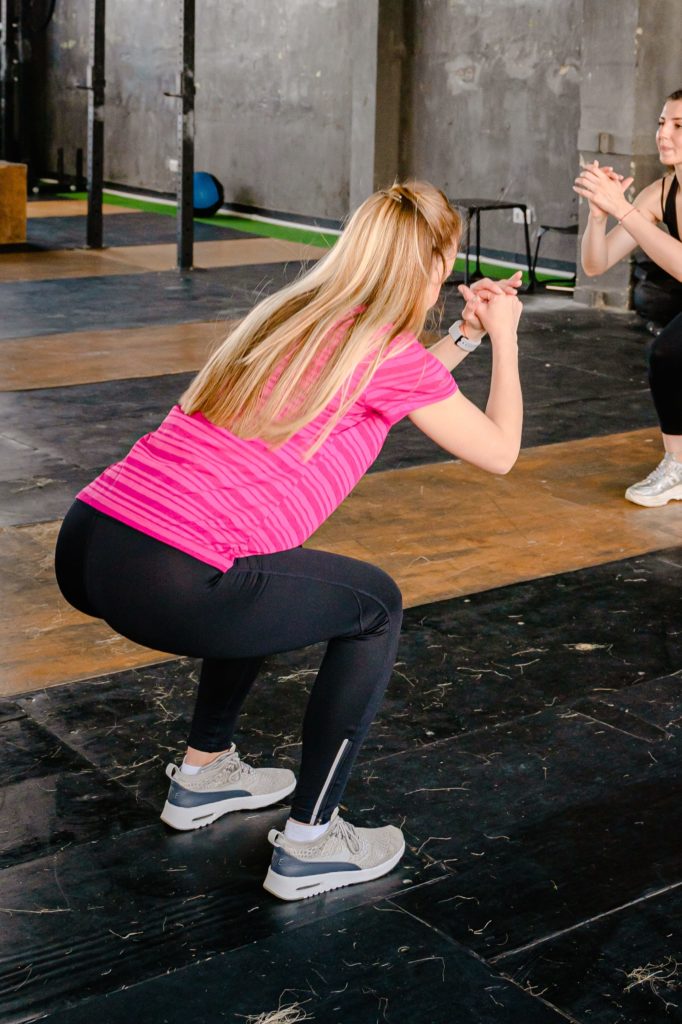
- Pelvic floor exercise 1: Lie on your back. Place your arms loosely on the floor, palms down. Wave your legs lightly. Now push your bottom up and stretch the groin towards the ceiling. Hold the position as long as you can. Now put down your butt and take a breather before repeating the exercise up to 5 times.
- Pelvic floor exercise 2: Tense the pelvic floor as if you wanted to crack a nut with your anus. Do you feel how the intestines, bladder and uterus lift? Then you’re doing it right. The rest of the posture is not important for this exercise, so you can practice it in the office, at the supermarket checkout and in business meetings.
- Pelvic floor exercise 3: Sit on a chair or bench at the very front of the edge of the seat. Your legs and knees are approximately at a right angle. Support yourself with your hands backwards and lean back slightly without touching the backrest. Raise your legs to keep them at right angles. In addition, tense the pelvic floor and stay in this position as long as you can.
Not only special exercises can prevent vaginal prolapse or uterine prolapse. Basically, holistic sports such as swimming, yoga, Pilates or fitness are suitable to strengthen the pelvic floor and the holding apparatus of the organs.
As a rule of thumb, butt exercises (e.g. properly performed squats) tend to be good for the pelvic floor, abdominal exercises and upper body exercises (e.g. sit-ups) tend to be bad for the holding apparatus of the abdomen because of the pressing force development in the abdomen.
Spinal disc herniation
Probably the best known prolapse is the intervertebral disc prolapse or herniated disc. The intervertebral discs are cartilage with a gelatinous core, which dampen shocks and friction between the vertebrae of the spine. They give the spine its mobility and have to perform very highly. With every step and every turn of the body, they are milled, compressed and pulled.
Prolapse can occur when an intervertebral disc is undersupplied, the load becomes too great or (genetically determined) malformations are present. The herniated disc usually has a history of years. Thus, it takes a long maldevelopment to damage the substance of the intervertebral disc to such an extent that it partially detaches from the neighboring vertebrae and penetrates into the spinal cord or peripheral area of the spine.
A herniated disc can be prevented primarily by building muscle and observing ergonomics at the workplace and in everyday life. Therapy in many cases is limited to treating the pain with medication and heat.
Hemorrhoids, anal and rectal prolapse
Haemorrhoids
Usually hemorrhoids mean a hemorrhoidal disease. Acute hemorrhoids complicate everyday life, because sitting becomes torment. And they violate the private sphere, because unpleasant visits to the doctor can hardly be avoided.
But what is it all about when we talk about hemorrhoids? Most often, hemorrhoids mean a lowering or prolapse of the vascular pads of the anus, which are called hemorrhoids. The hemorrhoids serve the fine sealing of the anus together with the sphincter, but in contrast are blood-filled vessels. They relax during bowel movements (emptying) and thus clear the way for emptying the rectum.
prolapse
If the hemorrhoids stand out, this occurs in gradations from mild and reversible (grade 1) to severe and irreversible (grade 4). Fourth-degree hemorrhoids are called prolapse and require treatment.
prolapse is considered a precursor of rectal prolapse, in which not only the mucous membranes in the area of the hemorrhoids of the anus emerge, but part of the rectum turns outwards.
In the early stages of hemorrhoids, patients and doctors prefer symptomatic treatment with ointments. They eliminate pain during bowel movements and reduce inflammation. However, in cases of pronounced prolapse, only surgery remains for healing. Thus, outpatient methods for the obliteration of hemorrhoids – for example, by means of syringes and by surgically placed rubber bands – have proven themselves.
Rectal prolapse
In later stages (hemorrhoids of the 4th degree) as well as in rectal prolapse, only inpatient surgical interventions bring healing. Here, excess tissue is removed, which is associated with significant risks in the case of rectal prolapse.
Differential diagnosis of prolapse
Depending on the type of prolapse, very different differential diagnoses are possible. Basically, cancers and tumors of the genital organs, the intestine or the organs in the chest and abdomen come into consideration. Also radiating spinal diseases, inflammation and injuries of soft tissues and the musculoskeletal system can trigger a feeling of pressure, pain and discomfort in the chest, back and abdomen.
In prolapse , a common differential diagnosis is thrombosis, a blood clot in a superficial vein in the anus that leads to painful swelling. The term thrombosis can be misleading in this case: In contrast to the dreaded deep vein thrombosis or other thrombi, thrombosis is usually harmless as often life-threatening circulatory disorders. The thrombus is broken down by the body within a few weeks.
The genital prolapse of the woman can manifest itself similar to an inguinal hernia (cf. hernia). In contrast to prolapse, this does not lower the vagina or uterus. The hernia is caused by a “hernia” in the abdominal wall or groin. Part of the intestine passes through this rupture, causing palpable, soft swelling. Like genital prolapse, the hernia is also favored by a weak supporting apparatus of ligaments and muscles as well as by strong efforts in the abdomen (pressing, incorrect lifting).
A herniated disc (the prolapse of an intervertebral disc) can be confused with other painful diseases of the spine, chest (thorax) and organs heart, lungs, kidneys and liver. Accident-related injuries and fractures of the spine also manifest themselves in comparable pain, but are rarely accompanied by disc prolapse. A herniated disc must therefore be detected by imaging techniques before the targeted therapy is initiated.
